Prevention, Screening, and Groundbreaking Research
As the days get warmer and longer, don’t forget about sun safety!
As a surgical oncologist specializing in treating melanoma and other skin cancers, I see firsthand how excess exposure to the sun’s UV rays can lead to a scary diagnosis.
The good news is that you can take steps to protect yourself and your family. Better screening and new research are making it possible to identify problems earlier.
Here’s what you need to know.
The key risk factor for melanoma and some other skin cancers is excess UV exposure from sunlight and tanning beds.
You probably know wearing sunscreen is essential, but how you apply it matters, too. I recommend an SPF of 50 or higher. Read the bottle and follow instructions for reapplying the product. Usually, you need to reapply every hour or two while in the sun, and more frequently when in the water.
Make sure you use enough to thoroughly cover your skin. Cover all exposed skin: face, ears, arms, legs, feet, hands, etc. Don’t forget easy-to-miss areas like scalp exposed by a part in your hair, the backs of your legs, and the tops of your feet and hands.
Being consistent can be easy! Many facial moisturizers include SPF, which is a great option for everyday protection.
For those who don’t like using sunscreen or have trouble remembering to reapply, you can also wear clothing with built-in UV protection. The fabric helps block damaging rays, and it’s an easy solution — you don’t have to remember to reapply! Wide-brimmed hats that shade your face and ears are convenient and can help you stay cool.
I always tell patients facing a new diagnosis that we can’t change the past. We can’t erase our cumulative sun exposure or childhood sunburns, but there’s a lot we can do to prevent future UV damage.
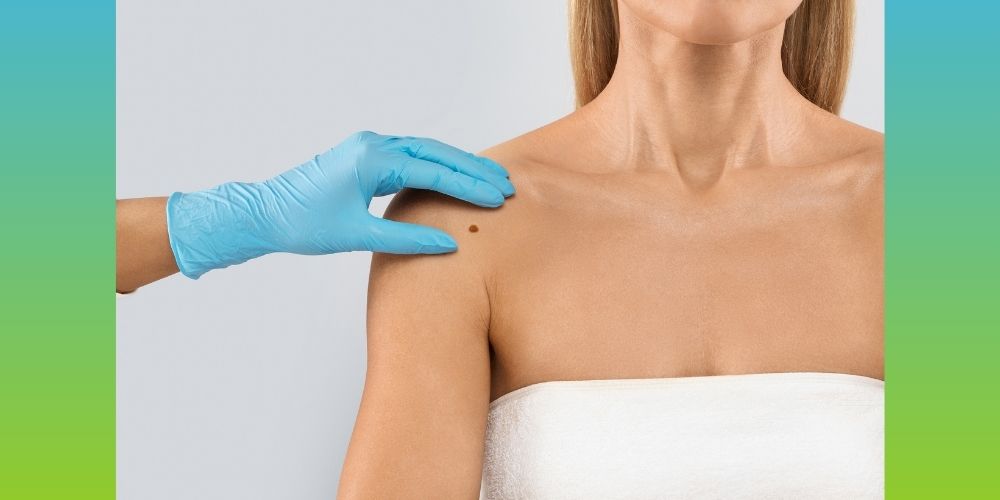
That’s where screening comes in. Proper screening can help catch melanomas and other skin cancers early.
The first step is being vigilant. Moles that are asymmetrical, feathered at the edges, a color other than light brown, or larger than a pencil eraser should be checked by a doctor. If a mole is growing or changing, it should also be checked.
We recommend annual full-body skin exams for patients starting in their 20s or 30s who have had significant sun exposure or tanning bed use, and more often if you’re high-risk due to family or personal history, very fair skin, or numerous moles.
Part of my research involves circulating tumor DNA, or ctDNA. This is a marker in the blood used in many other cancers that is now being studied in melanoma.
Our hope is that ctDNA can someday help us better predict the recurrence risk of melanomas. It may also help guide surveillance during or after melanoma has been treated.
At Regional One Health, we offer genetic counseling for eligible patients. For patients who test positive for genetic markers linked to hereditary melanoma, we discuss risk management options including lifestyle changes, enhanced screening, and preventive treatment.
Our team understands that cancer is scary, and we want to empower patients. By protecting your skin with clothing and SPF and being vigilant about screening, you can manage your risk and give yourself the best chance of catching problems early.
Visit Regionalonehealth.org/cancer-care for more information and call 901.515.HOPE (4673) for appointments.
Chelsea Olson, MD, DABS, is a surgical oncologist with Regional One Health Cancer Care. She sees patients at the Main Campus, 880 Madison Avenue, and the East Campus, 6555 Quince Road.
By Chelsea Olson, MD, DABS